Latarjet Procedure
The Latarjet Procedure is an operation used to treat anterior shoulder dislocations. The procedure was first described by French surgeon Dr. Michel Latarjet in 1954. The Latarjet Procedure is the most successful operation for shoulder anterior instability in preventing recurrence. It has been typically used in patients with glenoid and or humeral bone loss, failed soft tissue surgical procedures and contact athletes.
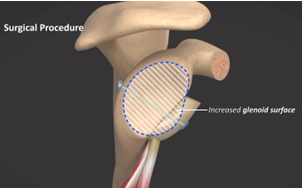
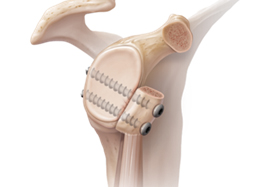
The Latarjet procedure involves transferring a piece of bone from the front of the shoulder blade (coracoid) and the attached tendons to the front of the shoulder socket (glenoid). It may be secured with screws or suture buttons. The shoulder ligaments are also repaired.
The procedure restores shoulder stability via 3 mechanisms:
- Restores socket bone
- The sling effect of the tendon, supporting the humeral head throughout the range of motion
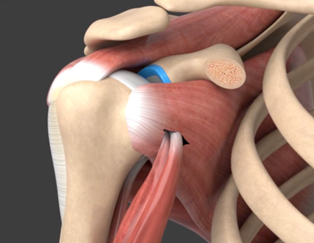
- Repairing the anterior shoulder capsule and ligaments, over the bone block
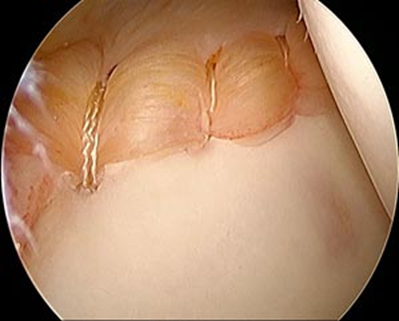
Latarjet Surgery and Recovery
The procedure takes approximately 90 mins. It is performed under a general anaesthesia with a nerve block to the arm. Most patients stay overnight and receive 24 hrs of antibiotics. A physiotherapist will show you the required exercises the morning after surgery. Surgical dressings are waterproof and can get wet in the shower. A combination of pain killers and ice is required for the first 3-5 days. Sling immobilisation is required for 6 weeks, including while sleeping. A range of motion program commences at 6 weeks and strength from 10 weeks.
Desk based work can commence while in the sling. Return to manual employment will have to be tailored, depending on driving requirements, the availability of light duties and required tasks. Contact sports can be resumed when strength, endurance and co-ordination are restored, usually after 6 months.
Appointments: occur in the rooms or via telehealth:
- Initial: Bring all investigations. A CT or MRI scan will be required to assess the shoulder.
- 2 weeks- wound check
- 6 weeks- check x-ray, remove sling, commence active ROM, organise physiotherapy
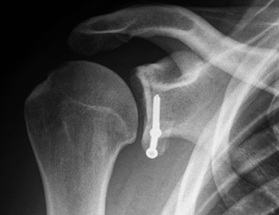 6 weeks X-ray
6 weeks X-ray - 16 weeks- discuss outcome and return to activity.
Results: The Latarjet procedure has the lowest recurrence of instability (3-5%) despite being used in more challenging cases. An arthroscopic stabilisation has recurrence rates long term of 10-15%. There may be a slight loss of movement, but the objective of the surgery is to stabilise and not tighten the shoulder. Shoulder instability causes joint surface damage, leading to an increased risk of shoulder arthritis. A well performed Latarjet Procedure should prevent further instability and limit arthritis progression.
Complications of the Latarjet procedure include:
- Infection: Rates are <1% and antibiotics are administered peri-operatively to reduce infection risk.
- Graft Issues: The graft may not unite to the socket, but this does not affect the operative results. Excess bone graft may resorb leading to screw prominence that can cause pain and require delayed screw removal.
- Nerve injury: Reported around 1-3%. The rare nerve injury is usually a nerve stretch that spontaneously recovers and does not require further surgery.
- Recurrent instability is rare and usually involves significant reinjury.
SUMMARY
The Latarjet procedure is an effective technique for restoring shoulder stability in individuals with bone loss, failed previous instability surgery and contact athletes.