Frozen Shoulder
What is the shoulder?
The shoulder is a complex ball-and-socket joint that allows full movement of the arm.
It offers a wide range of motion, but also makes it vulnerable to injury.
At the shoulder, three major bones meet and create a 90-degree angle. These bones are the
- collarbone (clavicle)
- the shoulder blade (scapula)
- humerus, the largest bone of the arm.
Three joints are formed from the junctions of these three bones and the sternum. These joints are the
- glenohumeral joint,
- acromioclavicular (AC) joint and
- sternoclavicular joint.
Each joint in the shoulder is surrounded by cartilage for padding, ligaments to connect the bonesand tendons to attach the muscles to the bones.
Each joint in the shoulder is surrounded by cartilage for padding, ligaments to connect the bones, muscles and tendons to attach the muscles to the bones.
What is Frozen Shoulder?
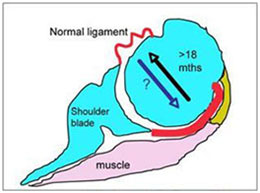
Frozen Shoulder (adhesive capsulitis) is a debilitating condition that causes acute shoulder pain and gradually increasing stiffness and loss of function. The pain and stiffness is caused by inflammation and thickening of the shoulder joint capsule and ligaments.The ligaments normally stabilize the shoulder but when inflamed and thickened, can cause severe pain on rapid movement and restrict movement in all directions. This makes it impossible for ladies to reach their bra strap with the affected arm. The shoulder pains begin slowly until there is significant loss of motion in the shoulder.
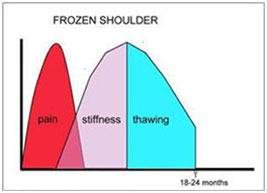
Typically the course of frozen shoulder lasts about 18-24 months . Rarely it can last up to 3 years. Frozen shoulder occurs in 3 overlapping stages:
- Painful stage - The patient develops a slow onset of pain. As the pain worsens, the shoulder starts to lose motion.
- Frozen stage - The patient experiences a slow improvement in pain, but the stiffness remains.
- Thawing stage - the patient slowly regains motion of their shoulder.
Causes of Frozen Shoulder:
Scientists are not sure what causes Frozen Shoulder. Frozen shoulder is common in patients who recently had to immobilize their shoulder for a long period after trauma, such as a shoulder fracture or surgery. Frozen shoulder without trauma is more frequently seen in middle aged women and patients with diabetes.
Other associations are:
- Thyroid disorders
- Heart Disease
- Parkinson’s Disease
Frozen Shoulder symptoms
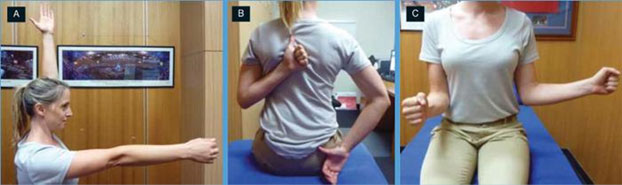
Frozen Shoulder may cause pain and sufferers have the following symptoms:
- Dull, aching Pain
- Sleep disturbance and deprivation
- Severe sharp pain with rapid movement (eg. trying to catch mobile phone)
- Difficulty with activities of daily living (eg. dressing, driving and personal care)
- Lack of movement in all directions
Diagnosis of Frozen Shoulder
Diagnostic methods include:
Consultation - During this consultation Dr Harper will:
- take a medical history: concentrating on pain, disability, treatments and associated medical conditions.
- perform a physical examination: documenting shoulder range of motion and strength.
Imaging tests -
- X-rays – Dense structures, such as bone, show up clearly on x-rays. The X-rays in non-traumatic frozen shoulder are usually normal. X-rays help exclude arthritis or other rare causes of shoulder pain and stiffnessi
- Ultrasound - can show the state of the rotator cuff tendons. Intact tendons in the setting of severe restriction in movement suggests frozen shoulder.
- MRI scans: are generally not required, reserved only for unusual cases.
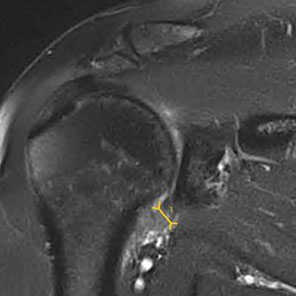
MRI scan showing thickened (5mm) inferior capsule (normally 1mm).
- While not all of these approaches or tests are required to confirm the diagnosis, this diagnostic process will also allow Dr Harper to review any possible risks or existing conditions that could interfere with recovery.
Treatment for Frozen Shoulder
Nonsurgical treatments can include:
Frozen shoulder generally improves over time, however it can take up to 3 years. With the favourable natural history of frozen shoulder being recovery of a pain-free functional shoulder, treatment is generally non-operative. Treatment includes:
- pain management: analgesics, Non-steroidal anti-inflammatory medication and image- guided Steroid injections into the ball and socket joint. An attempt to distend the shoulder joint with water (hydrodistension) can be combined with the steroid injection.
- minimising stiffness: Movement should be maintained with stretches while in the shower daily in all planes. Painful stretching should be avoided as this has been shown to increase the duration of the painful phase and lengthen the time to resolution.
- maintaining strength: Patients should maintain functional use and strength within the pain-free safe zone of movement.
Frozen Shoulder Surgery
Surgery for frozen shoulder is rarely required. It is more common in post-traumatic frozen shoulder that has not resolved within expected timeframes. The surgery involves cutting the tight ligaments and capsule and remove the scar tissue from the affected shoulder.
It can be performed with an arthroscope or with an open technique (larger incision). The primary advantage of arthroscopic technique is greater access to the front and back of joints without damage to normal structures.
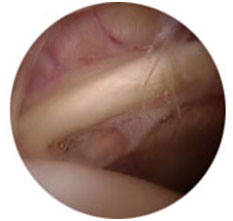 Normal joint lining (capsule)
Normal joint lining (capsule)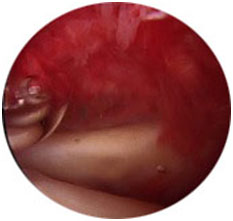 Frozen shoulder inflamed lining
Frozen shoulder inflamed lining
Arthroscopic division of capsule and ligaments
Frozen Shoulder Surgery Risks
As with any major surgery there are potential risks involved. The decision to proceed with the surgery is made because the advantages of surgery outweigh the potential disadvantages.
It is important that the patient is informed of these risks before the surgery takes place.
Complications can be medical (general) or specific to Arthroscopic capsular release surgery.
Medical complications include those of the anesthetic and your general well being. Almost any medical condition can occur so this list is not complete. Complications include:
- Allergic reactions to medications
- Heart attacks, strokes, kidney failure, pneumonia, bladder infections.
- Complications from nerve blocks such as infection or nerve damage.
- Blood Clots (Deep Venous Thrombosis) - Blood Clots can rarely form in the arm muscles and can travel to the lung (Pulmonary embolism). These can occasionally be serious and even life threatening. If the patient suffers arm pain, redness or swelling, or have shortness of breath at any stage, contact [doctor]
Serious medical problems can lead to ongoing health concerns, prolonged hospitalisation or rarely death.
Specific complications for surgery are rare but may include:
Infection - Infections can occur superficially at the incision or in the joint space of the shoulder, a more serious infection. Infection rates vary; if it occurs it can be treated with antibiotics but may require further surgery.
Shoulder Stiffness - Shoulder stiffness can recur despite capsular release surgical gains. It is crucial post-operatively to maximise pain management so that surgical gains in movement can be maintained with physiotherapy. This is very important in patients with co-existent chronic regional pain syndrome.
Dislocations - Dislocations and/or subluxations with activity can occur after dividing the ligaments that normally stabilise the joint.It is important that you follow your surgeon’s guidelines for activity restrictions.
Damage to nerves of Blood Vessels - Also rare but can lead to weakness or loss of sensation in part of the arm. Damage to blood vessels may require further surgery if bleeding is ongoing.
Damage to the joint - Joint damage to the cartilage or other structures can occur during surgery. The contracted shoulder capsule in frozen shoulder can make it very difficult to get into the ball and socket joint without scuffing cartilage.
Surgery Preparation
If surgery is required, preparation is necessary to achieve the best results and recovery.
Preparing mentally and physically for surgery is an important step toward a successful result.
- Dr Harper will outline the treatment plan and
- patients will need to understand the process and their participation.
Performing a tailored exercise program before surgery (ie. pre-hab) with a physiotherapist may assist with surgical recovery.
Dr Harper will also need to discuss:
- discuss any medications being taken with your doctor or physician to see which ones should be stopped before surgery
- do not eat or drink anything, including water, for 6 hours before surgery
- stop taking aspirin, warfarin, anti-inflammatory medications or drugs that increase the risk of bleeding one week before surgery to minimise bleeding
- stop or cut down smoking to reduce your surgery risks and improve your recovery
Post Shoulder Surgery
The patient will wake up in the recovery room and then be transferred back to their hospital room.
- Pain medication will be provided to keep the patient comfortable.
- A bandage will be around the operated shoulder and the arm will be in a sling The sling will be worn for comfort only and removed as soon as possible to encourage early restoration of shoulder motion
- Physiotherapy will be commenced in hospital and should be organised soon after discharge to maintain range of motion.
Dr Harper will see the patient prior to discharge and explain the findings of the operation and what was done during Surgery.
- The bandage will usually be removed the day after surgery and waterproof dressings applied by your nurse
- It is normal for the shoulder to swell after the surgery. Placing ice-packs on the shoulder will help to reduce swelling. Ice packs should be applied to the area for 20 min 3-4 times a day until swelling has reduced.
- 10-14 days after surgery Dr Harper will see the patient to monitor their progress and remove the sutures.
It is recommended that the patient not drive while wearing a sling due to safety reasons and the risk of injury to the surgical site.
The patient will be given specific instructions regarding activity and a rehabilitation program of exercise and strengthening.
Eating a healthy diet and not smoking will promote healing.





